They often had headaches and trouble sleeping. Like PCS patients, many members of the long-COVID group were brain-fogged and depressed. The cognitive neurologist Tamara Fong thought they resembled patients with post-concussive syndrome (PCS), which some neurologists hypothesize results from inflammation of the brain. Abramoff had never seen so many people with a single viral illness stay so impaired for so long.Īt Beth Israel Deaconess Medical Center in Boston, patients with milder COVID-19 began requesting help with mental fatigue and concentration problems late last year. Some began to get better after a couple of weeks or months, but a worrying minority remained ill. For some people, coordinating Zoom calls and emails was too much to handle. He said he sometimes felt disembodied-depersonalized, as if he were outside of himself.Īs these new patients-some 350 to date-arrived at the Penn clinic, Abramoff noticed the patterns now codified by Koralnik and his colleagues. Another man, a physician responsible for complex and nuanced diagnoses of heart patients, could not remember phrases that he used every day at work, such as blood pressure. His work involved keeping many things in his head at once, and he could no longer manage it. One man in his early 30s, whose physical COVID-19 symptoms had been limited to shortness of breath, appeared in Abramoff’s clinic in January, concerned about his ability to do his job. Read: ‘ICU delirium’ is leaving COVID-19 patients scared and confusedīut no one was prepared for the second wave of neurocognitive complaints, which came from people who had never been hospitalized. “A pneumonia patient in the ICU can be delirious,” Abramoff says. The sickest patients can experience hallucinations and psychoses. Many of those who survived with the help of ventilators emerged, expectedly, with “post-ICU syndrome,” a series of deficits that include memory, attention, and processing-speed impairments. 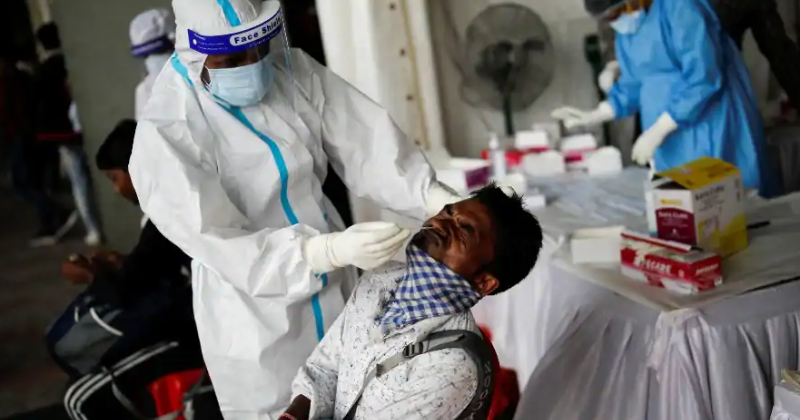
physicians, he was abruptly introduced to COVID-19 a year ago, when hospitals were inundated with critically ill patients-some of whom suffered brain damage from oxygen loss, blood clots, or strokes. Benjamin Abramoff, the director of Penn’s post-COVID clinic, is a physiatrist with a specialty in spinal-cord injury. While identifying long-COVID patients is challenging, helping them through the uncharted territory of their illness is more difficult still. Now, in the second year of the pandemic, researchers and therapists are beginning to understand how to help them. Like Gustafson, many of them are struggling with brain fog, and with its profound and often frightening disruptions to their daily lives. “It’s likely there are many millions of these patients in the U.S., and dozens of millions in the world,” Koralnik told me. That Koralnik’s study, like many of the new clinics, probably does not include many people without the resources or connections to find their way to specialized care only increases the uncertainty. “There’s no numerator or denominator for the group yet,” says Sara Manning, a neurologist at the new Post-COVID Assessment and Recovery Clinic at the University of Pennsylvania, one of dozens of such clinics springing up in the United States and worldwide. But official recognition doesn’t tell us what percentage of COVID-19 sufferers experience lingering neurocognitive problems, or how many long-COVID patients there are. In February, the National Institutes of Health gave long COVID a clinical name: Post-Acute Sequelae of SARS-CoV-2 infection (PASC). None had ever been hospitalized for COVID-19, yet 85 percent had four or more neurological complaints, including “brain fog”-persistent trouble with focusing, retaining short-term memories, and managing complex tasks. A just-published study led by Igor Koralnik, the director of the Neuro COVID-19 Clinic at Chicago’s Northwestern Memorial Hospital, analyzed the first 100 “long COVID” sufferers who came to the clinic, either in person or via virtual visits. The cognitive problems emerging from mild to moderate cases of COVID-19 are so new that researchers have struggled to define them. Before COVID-19, she’d held two part-time jobs, but she soon had to give up both of them. Once an avid reader, she couldn’t get through a page. Though her physical symptoms-diarrhea, dry cough, chills-were considered mild by doctors, her fatigue was crushing, and her mind was trapped in a fog. Debbie Gustafson of Dresher, Pennsylvania, was on the trip of a lifetime, touring the Galápagos with her family last March, when she began to feel the effects of COVID-19. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
